| 1851 | One person in four is killed by TB in Europe and America. | |||
| 1854 | TB is treated in sanatoria, with a strict regimen of bed rest, fresh air at all times – patients are even moved outside in their beds in all weathers – a healthy diet and a gradual increase in activity levels. | 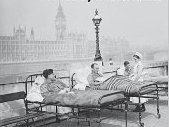 |
||
| 1882 | Robert Koch identifies that TB is caused by an organism, Mycobacterium tuberculosis. | |||
| 1919 |
The Housing Act is enacted in the UK, leading to slum clearance and a gradual improvement of living standards as new housing stock is built. Household overcrowding and transmission of TB is reduced. |  |
||
| 1920 | The first human trials of the vaccine Bacille Calmette-Guérin (BCG), an attenuated version of Mycobaterium bovis (Bovine TB), are launched. | |||
| 1935 | The Tuberculin Testing and Attested Herd Scheme, and increasing consumption of pasteurised milk, helps to prevent animal to human transmission of Bovine TB in the UK. |  |
||
| 1944 | Doctors Schatz, Bugie and Waksman announced the discovery of a drug called ‘Streptomycin‘ and that the first patient had been successfully treated with the drug. | |||
| 1952 | Doctors Robizek and Selikoff at Seaview Hospital, New York, use a new drug called ‘Isoniazid‘ to treat TB patients. |
|
||
| 1953 | A survey of 50,000 children showed an 80% reduction in infection rate following the BCG vaccination, leading to its introduction in secondary schools in the UK. At the time, those most at risk of TB in the UK were young adults in industrialised settings. The USA opts not to use BCG after their research showed contrary conclusions. | |||
| 1960 | Professor John Crofton, a TB expert at the University of Edinburgh, proposed that a combination of Streptomycin, PAS and Isoniazid, could completely cure TB if used from the outset of an individual case. This radical approach, which halved TB notifications in Edinburgh over a three year period, was initially met with disbelief. Sir John’s findings were soon replicated in a large scale international trial, leading to the introduction of combination therapy as the global gold standard treatment. This method, which became known as the “Edinburgh Method”, continues to influence the medical world today, including combined therapy for HIV. |  |
||
| 1970 | First outbreak of drug-resistant TB in the US. | |||
| 1987 | TB figures in England and Wales hit their lowest recorded level since records began – 5,745 cases – following a downward trend since the beginning of the century. This trend is set to reverse significantly in the following 25 years. |  |
||
| 1993 | The World Health Organization (WHO) declares TB ‘a global emergency’ with deaths from TB higher than any previous year in history. WHO estimates that one third of the world’s population is latently infected with TB, leading to 7-8 million cases of active TB – and 1.3-1.6 million deaths, annually. | |||
| 1995 | WHO begin promoting a new TB control strategy: Directly Observed Treatment Shortcourse (DOTS). DOTS features five components:
The first outbreak of multi-drug resistant TB (MDR-TB) is recorded in a London hospital HIV Unit. |
 |
||
| 1997 | India launches the Revised National Tuberculosis Control Programme (RNTCP), based on the DOTS strategy. India carries the burden of the highest number of TB cases in any one country. | |||
| 1999 | >> TB Alert, the UK’s national tuberculosis charity, launches on World TB Day, March 24th. |
|
||
| 2000 |
The Millennium Development Goals (MDGs) set a target to halt and begin to reverse the incidence of HIV, TB, malaria and other major diseases by 2015.
|
|||
| 2001 | The Stop TB Partnership is launched – with TB Alert as a founding partner – leading to the development of a Global Plan to Stop TB 2001-2006. | |||
| 2002 | The estimated global TB incidence rate peaks at 141 cases per 100,000 population. | |||
| 2003 | >> Archbishop Desmond Tutu becomes TB Alert’s Patron. He continues as Patron today, despite retiring from much of his charitable activities in 2011.
|
|||
| 2004 | The Chief Medical Officer publishes the TB action plan, Stopping Tuberculosis in England. TB Alert is a key stakeholder.
>> TB Alert India, TB Alert’s sister organisation, launches. |
|||
| 2005 | The number of deaths annually from TB peaks worldwide at 2 million. | |||
| 2006 | The second Global Plan to Stop TB (2006-2015) launches, setting out a revised blueprint for action to meet the targets set out under the first Global Plan.The National Institute for Health and Care Excellence (NICE) release new guidelines for TB in the UK: Clinical Diagnosis and Management of Tuberculosis, and Measures for its Prevention and Control, (2006). RESULTS-UK, with TB Alert’s support, set up an All Party Parliamentary Group on Global Tuberculosis to play a central role in focusing attention on TB in Westminster. | |||
| 2007 | The Department of Health launches Tuberculosis Prevention and Treatment: a toolkit for planning, commissioning and delivering high-quality services in England, in support of the 2004 TB action plan. |
|
||
| 2008 |
>> TB Alert develops The Truth About TB programme as the Department of Health’s lead partner in delivering its TB awareness raising objectives.
|
 |
||
| 2009 | The Third Partners’ Forum in Rio de Janeiro produces the Rio Recommendations on TB.
>> TB Alert’s Honorary President, Sir John Crofton, passes away peacefully at the age of 97. Having worked tirelessly, to the end, Sir John is attributed to having saved over 10 million lives from TB. He is sadly missed.
|
|||
| 2010 | Cepheid launch the Gene Xpert molecular test for TB. This rapid test is endorsed by WHO and hailed as a major breakthrough.The Stop TB Partnership launches the Global Plan to Stop TB 2011-2015. |  |
||
| 2011 | TB reaches a post-war peak in the UK – at 8,963 cases – though the overall trend indicates that levels have been stabilising since 2005. | |||
| 2012 | The Clinical Infectious Diseases Journal reports cases of totally drug-resistant TB (TDR-TB) in India. | |||